My name is Erin Sneed and I have been in the fitness industry for almost 10 years. I played sports all through high school and went on to play college soccer. While in college, I grew to love group fitness and began teaching classes at my college campus. I was extremely active and played pickup basketball, ran, taught workout classes, and trained on my own. In 2011, I was in the midst of my senior year of college and I began experiencing extreme hip pain. I shrugged it off and continued to workout daily, thinking I just needed to add more stretching to my routine. Little did I know I was running with a hip impingement and several labral tears which was putting the joint bone on bone and hip surgery recovery would be in my future.
About 6 months later, I couldn’t tolerate the pain anymore. I was 21 years old (at the time) and was waking up in the middle of night from the pain, unable to walk for more than 10 minutes without dragging my leg. I had acquired an extreme limp which caused every person to ask if I was ok.
Getting to the Bottom of the Issue
When I finally sought medical advice, I discovered that I had a congenital abnormality that causes a mismatch between the parts of the joint (the ball and socket) in the hip, and that, with my active lifestyle, had led to damage that could only be remedied with surgery. A total hip replacement was necessary, but not recommended due to my age.
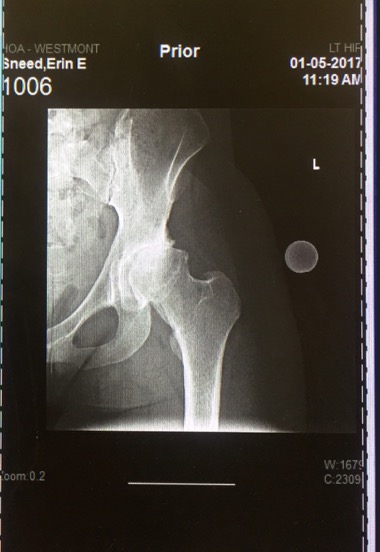
I learned that hip replacements don’t last forever and the more replacements a patient receives, the more difficult the recovery is. In 2012 I underwent my first hip surgery – an arthroscopic clean up of my joint to help relieve my pain and buy me some time before I had to have a total hip replacement.
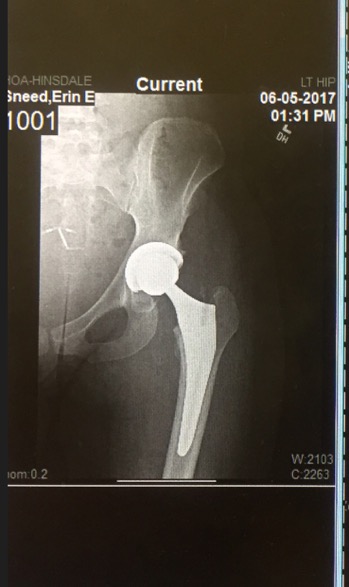
With any surgery, the recovery took a toll on my mind and body. I adjusted my workouts to more swimming, rollerblading, and cycling and removed running/impact training out of my routine. I became a cycling instructor and was back teaching in approximately 9 months. The arthroscopic surgery did relieve some pain; however, my range of motion did not recover. I only had 8 degrees of internal rotation in my surgical hip and retained a slight limp. Five years went by and and not only did my limp continue to become more and more pronounced, but the pain crept back into my life.
By this time, I had started a career in federal law enforcement and was gaining more popularity as a fitness professional in the city of Chicago. Going in for more hip issues was the last thing I wanted to do. I reluctantly went to the doctor who showed me my x-rays of an extremely arthritic hip and was surprised that I was even able to walk. A total hip replacement was strongly encouraged.
In my mind, the term “hip replacement” conjures up an image of a Baby Boomer keeping up with the grandkids, not a 26 year old just beginning her professional careers. I had now suffered from chronic hip pain for nearly 7 years and agreed to undergo the surgery with hopes of finally being pain free and without a limp.
As you can see from my video, I worked hard on my recovery and saw great results at first. I was finally living pain free and only had limitations of endurance walking, lateral movements, and running. I continued to attend physical therapy, which was recommended for 12 weeks.
Back to the Hip Surgery Recovery Drawing Board
About 4 months after my hip replacement, I began experiencing anterior hip pain (which was the same type of pain I had suffered from for years). I worked with my physical therapist to investigate what the issue could be and did some trial and error with exercises. I was beginning to limp again. I took a significant amount of time off from all physical activity which impacted my mind and body.
My physical therapist alluded that the pain and limp may have been from a weak gluteus medius and I began to train only that muscle (side steps, lateral leg raises, clam shells, hip abduction, etc.) for over a month. Despite my efforts, the pain persisted.
I scheduled an emergency appointment to see my surgeon who gave me a cortisone injection to relieve the pain. I had zero pain relief. I didn’t know what to do and began questioning if this limp and pain was something I was going to have forever. With a wedding around the corner in August 2018, my stress levels had risen. I had now not worked out in over 2 months and seemed to be out of options.
I doctor shopped, got a leg length discrepancy test done, and went to a different physical therapist to take a second look on what was going on and why I was feeling pain nearly 6 months post hip replacement. I had been doing my PT exercises and resting when needed. Fast-forward to over 32 weeks of physical therapy — which I was still continuing to attend several times weekly… the recommended amount for my surgery was 12 weeks.
A Second Set of Eyes
I went to see Jamie at NovaCare and she assessed my pain and checked my gluteus medius strength. I could hardly lift my leg it was so weak. How could this be?! I’d been doing gluteus medius exercises for over a month! Jamie watched and felt how I did my movements and informed me that YES, I was doing the exercises, BUT I was doing them with my hip flexor.
She explained that I have probably been moving incorrectly ever since my hip issues started and especially post hip surgery recovery – my body’s natural response to try to protect the hip joint was refusing to activate my gluteus medius and thus creating an over-activated hip flexor. She explained that I had no gluteus medius strength because my hip flexor had become the prime mover for ALL of my exercises, hence the anterior pain around my joint.
Jamie required me to take my physical therapy “back to basics” and only allowed me to do 2 exercises until I saw her next. In order to relieve the pain I needed to turn off my hip flexor and fire my side body. How do you turn off your hip flexor? You use it to walk, sit, lunge, etc. She assisted in turning off my hip flexor by doing some muscle relaxation techniques as well as dry needling.
For those of you who haven’t experienced dry needling, I’m not going to lie. Dry needling is unbelievably painful. However, it is also unbelievably effective. It’s a technique that is used to directly impact the muscle by moving the needle up and down that muscle or muscle group – allowing it go back to its relaxed state. In layman’s terms, it is a very intense version of foam rolling. Jamie said that by manually turning the hip flexor off I would have a better chance of firing the gluteus medius and over time strengthening it so it does the work it’s supposed to (stabilize the hip).
My Aha Moment

As someone who has been in the fitness industry this was such a powerful moment for me (and a total wakeup call). For many of us who enjoy working out, the easiest part about working out (believe it or not) is just grinding through your routine and getting the job done. However, I have learned the hard way that that’s not what fitness is about.
Yes working hard is great, but it’s about using the correct muscles to do the work you intend to do. If you’re doing a squat and you feel pain in your knees you may not be using the right muscles to do the work. My advice to anyone is to get a second set of eyes. Even if you think you’re doing an exercise correctly. If you are unsure about your form or have any doubts, get a second set of eyes to assist you! The power of a trainer, or in my case physical therapist, was life changing.
Post written by FFC Group Fitness Instructor Erin Sneed.
